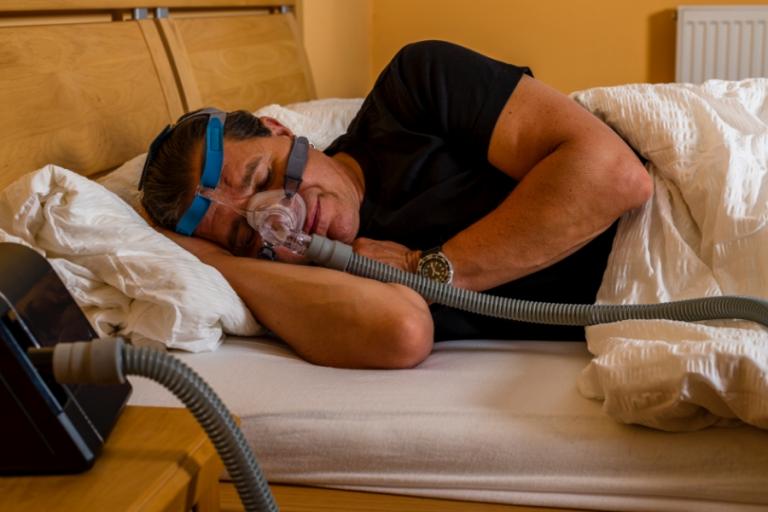
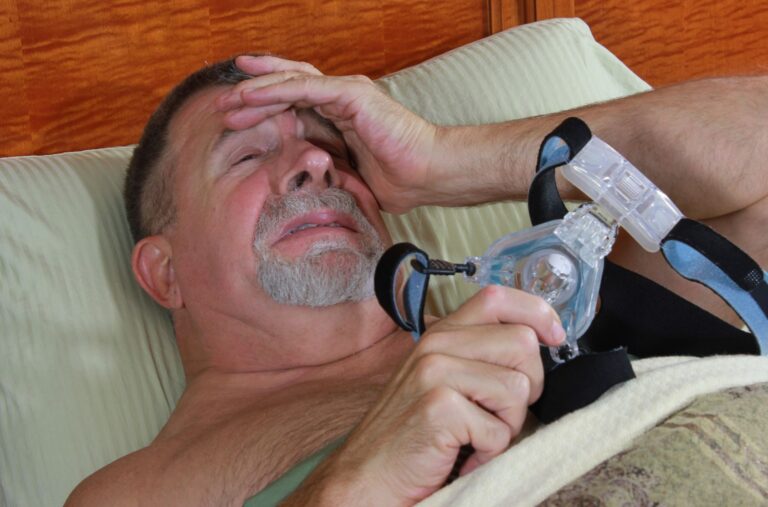
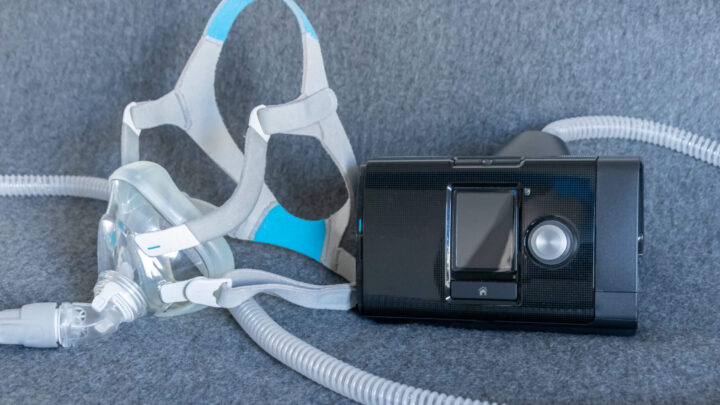
At Healthy Days, we are your dedicated resource for all things related to sleep apnea, CPAP machines, and CPAP/ResMed masks. Our mission is to help you achieve healthier, more restful nights of sleep, ensuring that each day is filled with vitality and well-being.